Here we discuss some common questions about joint injections.
What are joint injections?
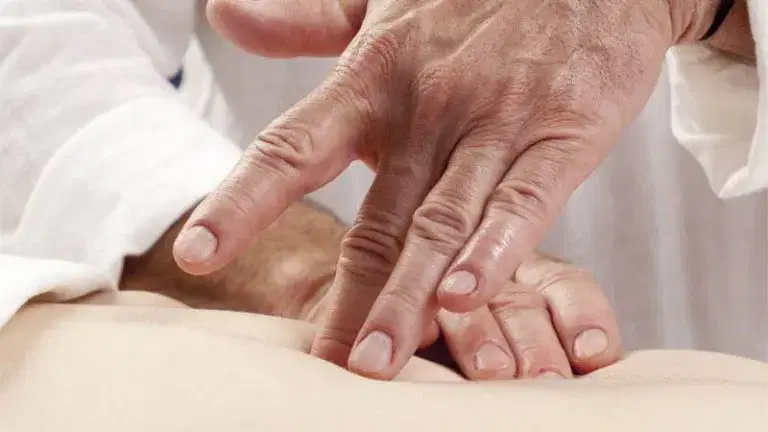
A joint injection is a procedure in which medication is applied via a syringe and needle directly into the space of your joints, such as your knee and hip joint. These are commonly done by doctors including surgeons and GPs, in clinics or hospitals.
Why do I need one?
If you have a joint which is painful, swollen, or you have difficulty with movement, you may benefit from a joint injection.
Your joint may be painful due to injury or a condition such as osteoarthritis or rheumatoid arthritis, tendinopathy, bursitis and other chronic (long term) joint problems. The intended effects are to reduce pain and improve the function of the joint so you can be more mobile.
If you need physiotherapy to improve your range of movement and mobility, injections can make it easier to do the exercises which will improve your joint strength.
What are the different types?
Steroids: The most common medication used is steroids such as hydrocortisone. Steroids work by reducing the inflammation in the joint which improves pain and mobility.
Viscosupplementation: Some may use hyaluronic acid instead of steroid injections. In osteoarthritis, the cartilage covering your bone in synovial joints wears down over time due to trauma or degeneration. Hyaluronic acid has a similar consistency to the synovial fluid found in the joints. Injecting hyaluronic acid viscosupplementation into the joint space aims to lubricate and therefore reduce pain caused by friction of bone on bone.
Platelet-rich plasma (PRP): PRP injections are used for patients with osteoarthritis and involves taking a component of your blood, called plasma, and injecting this into the joint. Your plasma contains factors which may both heal the damage within the joint by rebuilding cartilage and bone, and also may reduce inflammation. New technology means that only a small amount of your blood is taken and the PRP preparation can be created rapidly, so treatment is less expensive and has fewer healing complications. Tissue and bone grafts may also be incorporated. The whole procedure should take around an hour.
How are they performed on the hip and knee?
At your appointment, a specialist doctor such as an orthopaedic surgeon will give you your injection. Some doctors will administer a local anaesthetic injection before the injection into the skin, to prevent pain, and others will combine a local anaesthetic and the medication, so you only have to have one injection.
The doctor may use an ultrasound machine to scan the joint before inserting the needle. For hip and knee pain, you may need to lie down or sit up depending on the location. The procedure will usually take place in theatre with sterilised equipment.
What precautions do I need to take?
After the injection, you may have more pain initially before the steroids have time to work, and for this you should take painkillers and ice the joint. You should avoid driving yourself home from hospital or doing anything strenuous for five days after the procedure.
If you have health conditions such as diabetes, an infection, a bleeding disorder, or there is a risk you may be pregnant, you must inform your doctor of this before you have a joint injection.
What are the risks?
Local damage to the tendon, nerves, or bones can occur if the injection is not inserted correctly, as well as joint infection. A joint infection can occur due to bacteria entering the joint space and can lead to septic arthritis, where patients have a hot, red, swollen joint, and will need further treatment. It is possible to have an allergic reaction to the medication, but this is uncommon.
Steroids can suppress your immune system putting you more at risk of other infections. They are not thought to increase the risk of cornovirus infection based on the published evidence. Long term, they may cause further degeneration of the cartilage in your joint. Side effects of taking steroids may include mood changes, weight gain, thinning of skin and easy bruising, bone breakdown, and raised blood pressure or blood sugar.
How long do they last?
Usually the effects last several months although some patients report benefits for up to a year. For some, symptoms are alleviated with just one injection, but others require several injections. The injections may be repeated up to several times a year but having a joint injection more regularly than this can cause damage to your joint. Over time, the effectiveness of these injections may decrease.
Summary
It is important as a patient to understand the advantages and risks of having an injection for a painful joint and you are able to fully prepare for your procedure. If you wish to discuss this further please get in touch here or call 0161 772 0961 for further details.